Mental health issues in Canada - Statistics & Facts
Key insights
- Percentage of Canadians who perceived their mental health as very good or excellent
- 55%

Detailed statistics
Percent of Canadians perceiving mental health as very good or excellent 2003-2022
- Percentage of Canadians who reported being diagnosed with a mood disorder
- 11.4%

Detailed statistics
Percent of Canadians reported mood disorder diagnosis 2003-2022
- Number of suicides in Canada in 2021
- 3,769

Detailed statistics
Number of suicides Canada 2007-2021
Editor’s Picks Current statistics on this topic
Current statistics on this topic
Related topics
Recommended statistics
Mental health status
10
- Premium Statistic Leading health and wellness goals of Canadians 2020
- Basic Statistic Percent of Canadians perceiving strong sense of belonging to community 2003-2022
- Basic Statistic Percent of Canadians perceiving mental health as very good or excellent 2003-2022
- Premium Statistic Number of Canadians perceiving mental health as very good or excellent 2003-2022
- Basic Statistic Percent of Canadians perceiving mental health as fair or poor 2003-2022
- Basic Statistic Number of Canadians perceiving their mental health as fair or poor 2003-2022
- Premium Statistic Percent of Canadians reported mood disorder diagnosis 2003-2022
- Premium Statistic Number of Canadians reported mood disorder diagnosis 2003-2022
- Basic Statistic Elderly Canadians that had emotional distress in the past year, 2021, by province
- Premium Statistic Percentage of elderly Canadians had depression/anxiety as of 2021, by province
Mental health status
-
Premium Statistic
Leading health and wellness goals of Canadians 2020

Leading health and wellness goals of Canadians 2020
Top health and wellness goals and priorities of people in Canada in 2020
-
Basic Statistic
Percent of Canadians perceiving strong sense of belonging to community 2003-2022
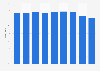
Percent of Canadians perceiving strong sense of belonging to community 2003-2022
Percentage of Canadians who have a somewhat or very strong sense of local community belonging from 2003 to 2022
-
Basic Statistic
Percent of Canadians perceiving mental health as very good or excellent 2003-2022

Percent of Canadians perceiving mental health as very good or excellent 2003-2022
Percentage of Canadians who perceived their mental health as very good or excellent from 2003 to 2022
-
Premium Statistic
Number of Canadians perceiving mental health as very good or excellent 2003-2022

Number of Canadians perceiving mental health as very good or excellent 2003-2022
Number of Canadians who perceived their mental health as very good or excellent from 2003 to 2022
-
Basic Statistic
Percent of Canadians perceiving mental health as fair or poor 2003-2022

Percent of Canadians perceiving mental health as fair or poor 2003-2022
Percentage of Canadians who perceived their mental health as fair or poor from 2003 to 2022
-
Basic Statistic
Number of Canadians perceiving their mental health as fair or poor 2003-2022

Number of Canadians perceiving their mental health as fair or poor 2003-2022
Number of Canadians who perceived their mental health as fair or poor from 2003 to 2022
-
Premium Statistic
Percent of Canadians reported mood disorder diagnosis 2003-2022

Percent of Canadians reported mood disorder diagnosis 2003-2022
Percentage of Canadians who reported being diagnosed with a mood disorder from 2003 to 2022
-
Premium Statistic
Number of Canadians reported mood disorder diagnosis 2003-2022

Number of Canadians reported mood disorder diagnosis 2003-2022
Number of Canadians who reported being diagnosed with a mood disorder from 2003 to 2022
-
Basic Statistic
Elderly Canadians that had emotional distress in the past year, 2021, by province
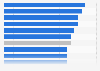
Elderly Canadians that had emotional distress in the past year, 2021, by province
Percentage of Canadian seniors aged 65 years and older that had experienced emotional distress within the past 12 months as of 2021, by province*
-
Premium Statistic
Percentage of elderly Canadians had depression/anxiety as of 2021, by province

Percentage of elderly Canadians had depression/anxiety as of 2021, by province
Share of Canadian seniors that had been told by a doctor they had depression, anxiety or another mental health condition as of 2021, by province
Treatment
8
- Basic Statistic Mental health care need perceived in Canada by age and gender 2018
- Premium Statistic Mental health care gap in Canada by province 2018
- Basic Statistic Share of adults in Canada who received mental health counseling in 2020, by province
- Basic Statistic Treatment methods used by Canadians with mood disorders, as of Dec. 2020
- Basic Statistic Conditions managed by medical cannabis among Canadian patients 2020
- Basic Statistic Share of Canadians open to allowing psilocybin-assisted psychotherapy in 2021
- Basic Statistic Number of Psychologists in Canada 2008-2021
- Basic Statistic Canadian nurses certifications by area of specialty 2022
Treatment
-
Basic Statistic
Mental health care need perceived in Canada by age and gender 2018

Mental health care need perceived in Canada by age and gender 2018
Percentage of Canada's population with perceived needs for mental health care in 2018, by age and gender
-
Premium Statistic
Mental health care gap in Canada by province 2018

Mental health care gap in Canada by province 2018
Percentage of Canada's population with perceived and unmet needs for mental health care in Canada 2018, by province*
-
Basic Statistic
Share of adults in Canada who received mental health counseling in 2020, by province

Share of adults in Canada who received mental health counseling in 2020, by province
Percentage of adults in Canada who received mental health counseling or treatment in the past year as of 2020, by province and territory
-
Basic Statistic
Treatment methods used by Canadians with mood disorders, as of Dec. 2020

Treatment methods used by Canadians with mood disorders, as of Dec. 2020
Mental health treatment methods used by Canadians diagnosed with depression, anxiety, or other mood disorders, as of December 2020
-
Basic Statistic
Conditions managed by medical cannabis among Canadian patients 2020

Conditions managed by medical cannabis among Canadian patients 2020
Percentage of Canadian patients who reported using medical cannabis for select conditions as of 2020
-
Basic Statistic
Share of Canadians open to allowing psilocybin-assisted psychotherapy in 2021

Share of Canadians open to allowing psilocybin-assisted psychotherapy in 2021
Percentage of Canadian adults who were open to Canadians being allowed to use psilocybin-assisted psychotherapy as part of their therapy as of 2021
-
Basic Statistic
Number of Psychologists in Canada 2008-2021

Number of Psychologists in Canada 2008-2021
Number of psychologists in Canada from 2008 to 2021
-
Basic Statistic
Canadian nurses certifications by area of specialty 2022
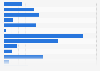
Canadian nurses certifications by area of specialty 2022
Number of valid nurse certifications in Canada in 2022, by area of specialty*
Costs
5
- Premium Statistic Mental health and addiction care costs in EDs in Canada in 2017-2018, by diagnosis
- Premium Statistic Cost for MHA stays in hospitals in Canada 2017-2018, by disorder
- Premium Statistic Spending per capita on mental health treatment in Canada 2017-2018, by territory
- Premium Statistic Health expenditure increases for mental health in Canada 2010-2018, by care setting
- Premium Statistic Increase in health expenditure for mental health in Canada 2010-2018, by territory
Costs
-
Premium Statistic
Mental health and addiction care costs in EDs in Canada in 2017-2018, by diagnosis

Mental health and addiction care costs in EDs in Canada in 2017-2018, by diagnosis
Total cost of mental health and addiction treatment in emergency departments in Canada in 2017-2018, by diagnosis (in million Canadian dollars)
-
Premium Statistic
Cost for MHA stays in hospitals in Canada 2017-2018, by disorder

Cost for MHA stays in hospitals in Canada 2017-2018, by disorder
Average cost of hospital stay for mental health disorders in Canada in 2017-2018, by disorder
-
Premium Statistic
Spending per capita on mental health treatment in Canada 2017-2018, by territory
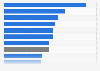
Spending per capita on mental health treatment in Canada 2017-2018, by territory
Average per capita spending on mental health and addiction (MHA) treatment in Canada in 2017-2018, by territory*
-
Premium Statistic
Health expenditure increases for mental health in Canada 2010-2018, by care setting
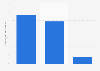
Health expenditure increases for mental health in Canada 2010-2018, by care setting
Percentage increase in public-sector health expenditure for mental health and addiction in Canada 2010 vs. 2018, by care setting*
-
Premium Statistic
Increase in health expenditure for mental health in Canada 2010-2018, by territory
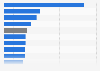
Increase in health expenditure for mental health in Canada 2010-2018, by territory
Percentage increase in public-sector health expenditure for mental health and addiction in Canada 2010 vs. 2018, by territory
Suicide
7
- Basic Statistic Prevalence of suicidal ideation among Canadian adults in 2019 and 2021, by age
- Premium Statistic Prevalence of suicidal ideation among Canadian adults in 2019 and 2021, by income
- Basic Statistic Prevalence of suicidal ideation among Canadian adults in 2019 and 2021, by province
- Basic Statistic Number of suicides Canada 2007-2021
- Premium Statistic Death rate for intentional self-harm (suicide) in Canada 2000-2022
- Basic Statistic Number of suicides Canada by age group 2021
- Basic Statistic Rate of suicide Canada by age group 2021
Suicide
-
Basic Statistic
Prevalence of suicidal ideation among Canadian adults in 2019 and 2021, by age

Prevalence of suicidal ideation among Canadian adults in 2019 and 2021, by age
Share of adults in Canada with suicidal ideation in the past 12 months in 2019 and 2021, by age
-
Premium Statistic
Prevalence of suicidal ideation among Canadian adults in 2019 and 2021, by income

Prevalence of suicidal ideation among Canadian adults in 2019 and 2021, by income
Share of adults in Canada with suicidal ideation in the past 12 months in 2019 and 2021, by income
-
Basic Statistic
Prevalence of suicidal ideation among Canadian adults in 2019 and 2021, by province

Prevalence of suicidal ideation among Canadian adults in 2019 and 2021, by province
Share of adults in Canada with suicidal ideation in the past 12 months in 2019 and 2021, by province
-
Basic Statistic
Number of suicides Canada 2007-2021

Number of suicides Canada 2007-2021
Number of suicides in Canada from 2007 to 2021*
-
Premium Statistic
Death rate for intentional self-harm (suicide) in Canada 2000-2022

Death rate for intentional self-harm (suicide) in Canada 2000-2022
Death rate for intentional self-harm (suicide) in Canada from 2000 to 2022 (per 100,000 population)
-
Basic Statistic
Number of suicides Canada by age group 2021

Number of suicides Canada by age group 2021
Number of suicides in Canada by age group in 2021
-
Basic Statistic
Rate of suicide Canada by age group 2021

Rate of suicide Canada by age group 2021
Suicide rate in Canada by age group in 2021 (per 100,000 population)
Focus: Mental health and the COVID-19 pandemic
8
- Basic Statistic Loneliness, anxiety, trouble sleeping among Canadians due to COVID-19 as of March 24
- Basic Statistic Canadian adult stress levels before and after COVID-19 outbreak as of April 27, 2020
- Basic Statistic Mental stress changes among Canadians, April 2020 to January 2021, by month
- Basic Statistic Anxiety in Canadians before/since the COVID-19 pandemic as of Dec. 2020, by province
- Basic Statistic Canadians' depression before/since the COVID-19 pandemic as of Dec. 2020, by province
- Basic Statistic Mood disorders among Canadians before/since the COVID-19 pandemic, as of Dec. 2020
- Premium Statistic Indigenous Canadians who reported worsening of mental health due to COVID as of 2020
- Basic Statistic Mental health supports in Canada before/since the COVID-19 pandemic, as of Dec. 2020
Focus: Mental health and the COVID-19 pandemic
-
Basic Statistic
Loneliness, anxiety, trouble sleeping among Canadians due to COVID-19 as of March 24

Loneliness, anxiety, trouble sleeping among Canadians due to COVID-19 as of March 24
Percentage of Canadian adults who had select feelings as a result of coronavirus (COVID-19) in the past week as of March 24, 2020
-
Basic Statistic
Canadian adult stress levels before and after COVID-19 outbreak as of April 27, 2020

Canadian adult stress levels before and after COVID-19 outbreak as of April 27, 2020
Level of stress felt by Canadians in the month previous to the COVID-19 outbreak and the last month April 27, 2020
-
Basic Statistic
Mental stress changes among Canadians, April 2020 to January 2021, by month

Mental stress changes among Canadians, April 2020 to January 2021, by month
Changes in mental stress among Canadians from April 2020 to January 2021, by month
-
Basic Statistic
Anxiety in Canadians before/since the COVID-19 pandemic as of Dec. 2020, by province

Anxiety in Canadians before/since the COVID-19 pandemic as of Dec. 2020, by province
Percentage of Canadians experiencing high levels of anxiety before or since the COVID-19 outbreak as of December 2020, by province
-
Basic Statistic
Canadians' depression before/since the COVID-19 pandemic as of Dec. 2020, by province

Canadians' depression before/since the COVID-19 pandemic as of Dec. 2020, by province
Percentage of Canadians experiencing high levels of depression before or since the COVID-19 outbreak as of December 2020, by province
-
Basic Statistic
Mood disorders among Canadians before/since the COVID-19 pandemic, as of Dec. 2020

Mood disorders among Canadians before/since the COVID-19 pandemic, as of Dec. 2020
Percentage of Canadians diagnosed with mood disorders before or since the COVID-19 outbreak, as of December 2020
-
Premium Statistic
Indigenous Canadians who reported worsening of mental health due to COVID as of 2020

Indigenous Canadians who reported worsening of mental health due to COVID as of 2020
Percentage of indigenous people in Canada with long-term conditions/disabilities who reported a worsening of mental health since the start of the COVID-19 pandemic in 2020*
-
Basic Statistic
Mental health supports in Canada before/since the COVID-19 pandemic, as of Dec. 2020

Mental health supports in Canada before/since the COVID-19 pandemic, as of Dec. 2020
Percentage of Canadians accessing mental health supports before or since the COVID-19 outbreak as of December 2020, by type of support
Further reportsGet the best reports to understand your industry
Get the best reports to understand your industry
Contact


Mon - Fri, 9am - 6pm (EST)
Mon - Fri, 9am - 5pm (SGT)
Mon - Fri, 10:00am - 6:00pm (JST)
Mon - Fri, 9:30am - 5pm (GMT)
Mon - Fri, 9am - 6pm (EST)





